Page 6 - CUAJ April 2019: Surveillance urodynamics for neurogenic lower urinary tract dysfunction: A systematic review
P. 6
Kavanagh et al
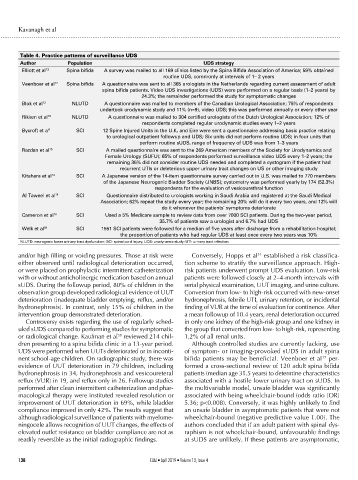
Table 4. Practice patterns of surveillance UDS
Author Population UDS strategy
Elliott et al 13 Spina bifida A survey was mailed to all 169 clinics listed by the Spina Bifida Association of America; 59% obtained
routine UDS, commonly at intervals of 1– 2 years
Veenboer et al 17 Spina bifida A questionnaire was sent to all 365 urologists in the Netherlands regarding current assessment of adult
spina bifida patients. Video UDS investigations (UDS) were performed on a regular basis (1–2 years) by
24.3%; the remainder performed the study for symptomatic changes
Blok et al 12 NLUTD A questionnaire was mailed to members of the Canadian Urological Association; 75% of respondents
undertook urodynamic study and 11% (n=9), video UDS; this was performed annually or every other year
Rikken et al 16 NLUTD A questionnaire was mailed to 304 certified urologists of the Dutch Urological Association; 12% of
respondents completed regular urodynamic studies every 1–2 years
Bycroft et a l4 SCI 12 Spine Injured Units in the U.K. and Eire were sent a questionnaire addressing basic practice relating
to urological outpatient followup and UDS; Six units did not perform routine UDS; in four units that
perform routine sUDS, range of frequency of UDS was from 1–3 years
Razdan et al 15 SCI A mailed questionnaire was sent to the 269 American members of the Society for Urodynamics and
Female Urology (SUFU); 65% of respondents performed surveillance video UDS every 1–2 years; the
remaining 35% did not consider routine UDS needed and completed a cystogram if the patient had
recurrent UTIs or deleterious upper urinary tract changes on US or other imaging study
Kitahara et al 14 SCI A Japanese version of the 14-item questionnaire survey carried out in U.S. was mailed to 770 members
of the Japanese Neurogenic Bladder Society (JNBS); cystometry was performed yearly by 174 (52.3%)
respondents for the evaluation of vesicourethral function
Al Taweel et al 11 SCI Questionnaire distributed to urologists working in Saudi Arabia and registered at the Saudi Medical
Association; 62% repeat the study every year; the remaining 20% will do it every two years, and 12% will
do it whenever the patients’ symptoms deteriorate
Cameron et al 18 SCI Used a 5% Medicare sample to review data from over 7000 SCI patients. During the two-year period,
35.7% of patients saw a urologist and 6.7% had UDS
Welk et al 19 SCI 1551 SCI patients were followed for a median of five years after discharge from a rehabilitation hospital;
the proportion of patients who had regular UDS at least once every two years was 10%
NLUTD: neurogenic lower urinary tract dysfunction; SCI: spinal cord injury; UDS: urodynamic study; UTI: urinary tract infection.
and/or high filling or voiding pressures. Those at risk were Conversely, Hopps et al established a risk classifica-
31
either observed until radiological deterioration occurred, tion scheme to stratify the surveillance approach. High-
or were placed on prophylactic intermittent catheterization risk patients underwent prompt UDS evaluation. Low-risk
with or without anticholinergic medication based on annual patients were followed closely at 2–4-month intervals with
sUDS. During the followup period, 80% of children in the serial physical examination, UUT imaging, and urine culture.
observation group developed radiological evidence of UUT Conversion from low- to high-risk occurred with new-onset
deterioration (inadequate bladder emptying, reflux, and/or hydronephrosis, febrile UTI, urinary retention, or incidental
hydronephrosis). In contrast, only 15% of children in the finding of VUR at the time of evaluation for continence. After
intervention group demonstrated deterioration. a mean followup of 10.4 years, renal deterioration occurred
Controversy exists regarding the use of regularly sched- in only one kidney of the high-risk group and one kidney in
uled sUDS compared to performing studies for symptomatic the group that converted from low- to high-risk, representing
or radiological change. Kaufman et al reviewed 214 chil- 1.2% of all renal units.
30
dren presenting to a spina bifida clinic in a 13-year period. Although controlled studies are currently lacking, use
UDS were performed when UUTs deteriorated or in inconti- of symptom- or imaging-provoked sUDS in adult spina
17
nent school-age children. On radiographic study, there was bifida patients may be beneficial. Veenboer et al per-
evidence of UUT deterioration in 79 children, including formed a cross-sectional review of 120 adult spina bifida
hydronephrosis in 34, hydronephrosis and vesicoureteral patients (median age 31.5 years) to determine characteristics
reflux (VUR) in 19, and reflux only in 26. Followup studies associated with a hostile lower urinary tract on sUDS. In
performed after clean intermittent catheterization and phar- the multivariable model, unsafe bladder was significantly
macological therapy were instituted revealed resolution or associated with being wheelchair-bound (odds ratio [OR]
improvement of UUT deterioration in 69%, while bladder 5.36; p<0.008). Conversely, it was highly unlikely to find
compliance improved in only 42%. The results suggest that an unsafe bladder in asymptomatic patients that were not
although radiological surveillance of patients with myelome- wheelchair-bound (negative predictive value 1.00). The
ningocele allows recognition of UUT changes, the effects of authors concluded that if an adult patient with spinal dys-
elevated outlet resistance on bladder compliance are not as raphism is not wheelchair-bound, unfavourable findings
readily reversible as the initial radiographic findings. at sUDS are unlikely. If these patients are asymptomatic,
138 CUAJ • April 2019 • Volume 13, Issue 4