Page 9 - CANADIAN URINARY DIVERSIONS POSITION STATEMENT
P. 9
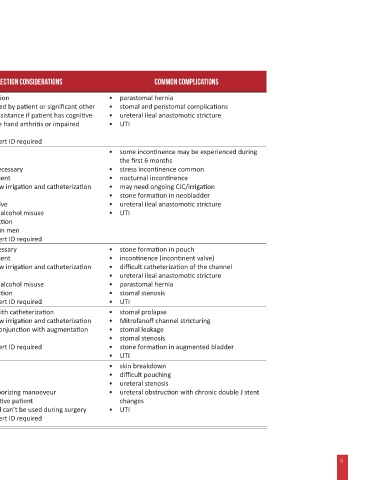
Table 1 Quick reference guide to the five urinary diversions
Continent/ Preop site Requires
Incontinent Ostomy marking CIC Patient selection considerations Common complications
Ileal conduit Incontinent Yes Yes No • most common diversion • parastomal hernia
• some dexterity needed by patient or significant other • stomal and peristomal complications
• may need ongoing assistance if patient has cognitive • ureteral ileal anastomotic stricture
deficiencies or severe hand arthritis or impaired • UTI
eyesight
• wearing a medical alert ID required
Orthotopic Continent No Yes Depends • common diversion • some incontinence may be experienced during
neobladder • esthetic preference the first 6 months
(for placement site of • dexterity for CIC is necessary • stress incontinence common
temporary suprapubic • no cognitive impairment • nocturnal incontinence
catheter or if intraoperative • commitment to follow irrigation and catheterization • may need ongoing CIC/irrigation
decision to proceed with schedule • stone formation in neobladder
an ileal conduit) • ability to problem solve • ureteral ileal anastomotic stricture
• no history of drug or alcohol misuse • UTI
• need good renal function
• fewer complications in men
• wearing a medical alert ID required
Indiana pouch Continent Yes Yes Yes • dexterity for CIC necessary • stone formation in pouch
• no cognitive impairment • incontinence (incontinent valve)
• commitment to follow irrigation and catheterization • difficult catheterization of the channel
schedule • ureteral ileal anastomotic stricture
• no history of drug or alcohol misuse • parastomal hernia
• need good renal function • stomal stenosis
• wearing a medical alert ID required • UTI
Mitrofanoff Continent Yes Yes Yes • must be compliant with catheterization • stomal prolapse
• commitment to follow irrigation and catheterization • Mitrofanoff channel stricturing
schedule if done in conjunction with augmentation • stomal leakage
cystoplasty • stomal stenosis
• wearing a medical alert ID required • stone formation in augmented bladder
• UTI
Cutaneous Incontinent No Yes No • least common • skin breakdown
ureterostomy • less invasive • difficult pouching
Stents • elderly & palliative • ureteral stenosis
present • paediatrics as a temporizing manoeveur • ureteral obstruction with chronic double J stent
• palliate the non-curative patient changes
• consider when bowel can’t be used during surgery • UTI
• wearing a medical alert ID required
Note. CIC=clean intermittent catheterization, UTI=urinary tract infection
CANADIAN URINARY DIVERSIONs POSITION STATEMENT 8