Page 8 - CUA 2020_Functional Urology
P. 8
Unmoderated Posters 3: Prostate Cancer, Functional Urology, Other Urology Topics
UP-3.9. Table 2. Univariable and multivariable association for recurrence-free survival
Recurrence-free survival (univariate) Recurrence-free survival (multivariate)
Parameter Hazard ratio 95% hazard ratio p Hazard ratio 95% hazard ratio p
confidence confidence
Limits Limits
Tumor grade 2.77 2.29 3.35 <0.0001 2.04 2.04 2.86 <0.0001
Tumor margin 3.06 2.28 4.11 <0.0001 2.15 1.62 2,86 <0.0001
Tumor size 1.05 1.03 1.07 <0.0001 1.05 1.03 1.06 <0.0001
Adrenalectomy 1.5 1.23 1.82 <0.0001 1.07 0.85 1.35 0.55
Conclusions: In this contemporary cohort, incidental adrenalectomy standard computerized tomography (CT) or magnetic resonance imaging
was not associated with better outcomes and likely reflect the more (MRI) have adequately identified IVC extension, however, proximal extent
advanced disease characteristics in this group. Adrenal sparing surgery can be underestimated. Accurate and timely assessment of tumor thrombus
should remain the standard of care when technically feasible and in the staging is imperative prior to undertaking radical surgical resection. We
absence of imaging abnormalities. aimed to assess the value of dual energy CT in the evaluation of IVC tumor
References thrombus in patients undergoing nephrectomy and IVC thrombectomy.
1. Leibovitch I, Raviv G, Mor Y, et al. Reconsidering the necessity Methods: Four patients identified to have resectable IVC thrombus were
of ipsilateral adrenalectomy during radical nephrectomy for renal included in the pilot study. All patients had undergone standard CT at
cell carcinoma. Urology 1995;46:316-20. https://doi.org/10.1016/ external imaging services and were reviewed independently. Contrast-
S0090-4295(99)80213-1 enhanced dual-energy CT was subsequently performed within seven days
2. Weight CJ, Kim SP, Lohse CM, et al. Routine adrenalectomy in prior to planned resection using an adapted CT protocol. Virtual unen-
patients with locally advanced renal cell cancer does not offer hancement, blended-weighted average, and color-coded iodine overlay
oncologic benefit and places a significant portion of patients at reconstruction was performed. All images were then re-analyzed by a radi-
risk for an asynchronous metastasis in a solitary adrenal gland. Eur ologist, urologist, and trainee who were unaware of the original reports.
Urol 2011;60:458-64. https://doi.org/10.1016/j.eururo.2011.04.022 Final determination of tumor thrombus level was made by consensus
3. Yap SA, Alibhai SMH, Abouassaly R, et al. Ipsilateral adrenalectomy following intraoperative findings.
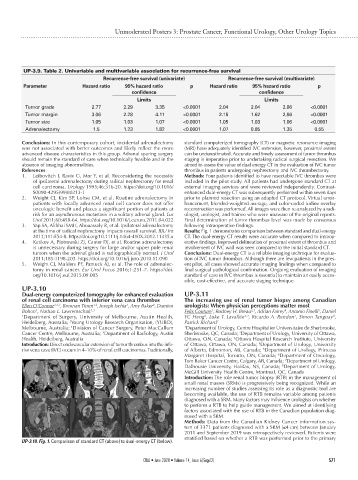
at the time of radical nephrectomy impacts overall survival. BJU Int Results: Fig. 1 demonstrates comparison between standard and dual-energy
2013;111:E54-8. https://doi.org/10.1111/j.1464-410X.2012.11435.x CT. The dual-energy CT results were accurate when compared to intraop-
4. Kutikov A, Piotrowski ZJ, Canter DJ, et al. Routine adrenalectomy erative findings. Improved delineation of proximal extent of thrombus and
is unnecessary during surgery for large and/or upper pole renal involvement of IVC wall was seen compared to the initial standard CT.
tumors when the adrenal gland is radiographically normal. J Urol Conclusions: Dual-energy CT is a reliable imaging technique for evalua-
2011;185:1198-203. https://doi.org/10.1016/j.juro.2010.11.090 tion of IVC tumor thrombus. Although there are few patients in the pres-
5. Weight CJ, Mulders PF, Pantuck AJ, et al. The role of adrenalec- ent pilot, all cases showed accurate imaging findings when compared to
tomy in renal cancer. Eur Urol Focus 2016;1:251-7. https://doi. final surgical pathological confirmation. Ongoing evaluation of imaging
org/10.1016/j.euf.2015.09.005 standard of care in IVC thrombus is essential to maintain an easily acces-
sible, cost-effective, and accurate staging technique.
UP-3.10
Dual-energy computerized tomography for enhanced evaluation UP-3.11
of renal cell carcinoma with inferior vena cava thrombus The increasing use of renal tumor biopsy among Canadian
Ellen O’Connor 1,2,3 , Brennan Timm , Joseph Ischia , Amy Baker , Damien urologists: When physician perceptions matter most
4
1,2
1
2,3
1
5
4
1
Bolton , Nathan L. Lawrentschuk 1,3 Felix Couture , Rodney H. Breau , Adrian Fairey , Antonio Finelli , Daniel
7
1 Department of Surgery, University of Melbourne, Austin Health, YC Heng , Luke T. Lavallée , Ricardo A. Rendon , Simon Tanguay ,
8
2,3
6
2
Heidelberg, Australia; Young Urology Research Organisation, (YURO), Patrick Richard 1
Melbourne, Australia; Division of Cancer Surgery, Peter MacCallum 1 Department of Urology, Centre Hospitalier Universitaire de Sherbrooke,
3
2
Cancer Centre, Melbourne, Australia; Department of Radiology, Austin Sherbrooke, QC, Canada; Department of Urology, University of Ottawa,
4
Health, Heidelberg, Australia Ottawa, ON, Canada; Ottawa Hospital Research Institute, University
3
Introduction: Direct endovascular extension of tumor thrombus into the infe- of Ottawa, Ottawa, ON, Canada; Department of Urology, University
4
5
rior vena cava (IVC) occurs in 4–10% of renal cell carcinomas. Traditionally, of Alberta, Edmonton, AB, Canada; Department of Urology, Princess
Margaret Hospital, Toronto, ON, Canada; Department of Oncology,
6
Tom Baker Cancer Centre, Calgary, AB, Canada; Department of Urology,
7
Dalhousie University, Halifax, NS, Canada; Department of Urology,
8
McGill University Health Centre, Montreal, QC, Canada
Introduction: The role renal tumor biopsy (RTB) in the management of
small renal masses (SRMs) is progressively being recognized. While an
increasing number of studies assessing its role as a diagnostic tool are
becoming available, the use of RTB remains variable among patients
diagnosed with a SRM. Many factors may influence urologists on whether
to perform a RTB to help guide management. We aimed at identifying
factors associated with the use of RTB in the Canadian population diag-
nosed with a SRM.
Methods: Data from the Canadian Kidney Cancer information sys-
tem of 3371 patients diagnosed with a SRM (≤4 cm) between January
2011 and September 2019 was retrospectively reviewed. Patients were
stratified based on whether a RTB was performed prior to the primary
UP-3.10. Fig. 1. Comparison of standard CT (above) to dual-energy CT (below).
CUAJ • June 2020 • Volume 14, Issue 6(Suppl2) S71